Contents
- What Is Venous Stasis Dermatitis?
- Why Poor Circulation Triggers Skin Changes
- Stages of Venous Stasis Dermatitis
- Common Symptoms of Venous Stasis Dermatitis
- Most Common Causes of Venous Stasis Dermatitis
- How a Vein Specialist Helps Manage Venous Stasis Dermatitis
- Why Early Treatment Makes a Difference
- Frequently Asked Questions
- Take the Next Step Toward Healthier Legs
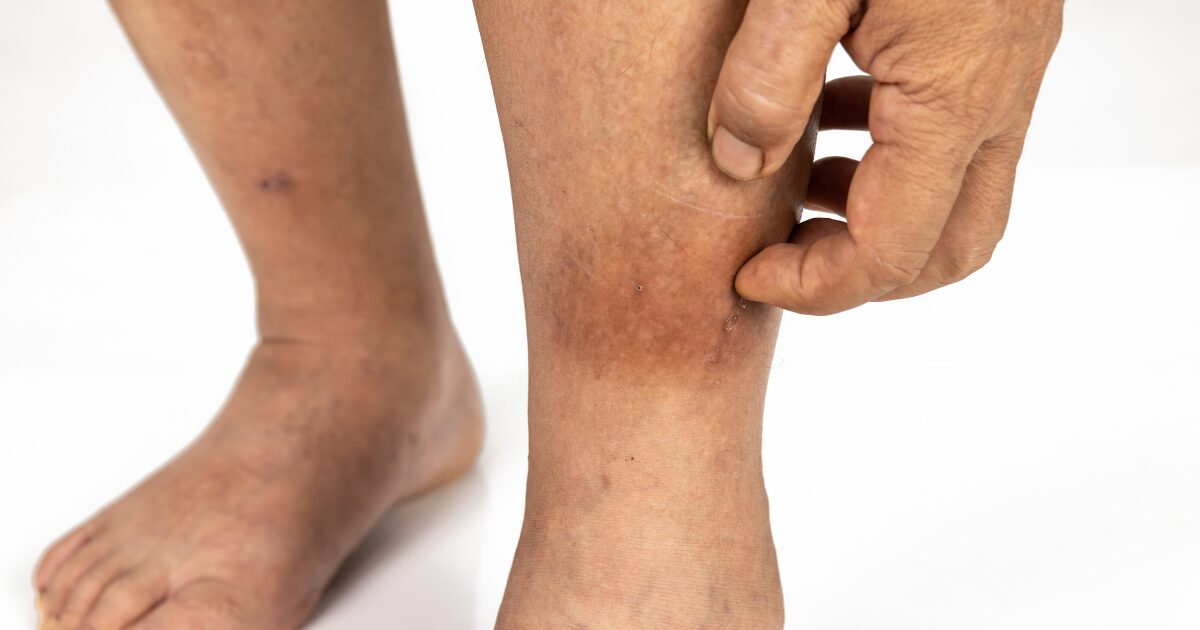
Skin changes on the lower legs are easy to dismiss at first. A little discoloration. Some itchiness. Swelling that comes and goes. But when these symptoms linger or worsen, they may point to something deeper than a skin issue alone.
Venous stasis dermatitis is a visible sign of an underlying circulation problem. It develops when blood flow in the legs is not working as it should, leading to pressure buildup inside the veins. Over time, that pressure affects the surrounding tissue and skin, causing inflammation, irritation, and sometimes painful wounds.
Understanding what causes venous stasis dermatitis, how it progresses, and when to seek care can make a meaningful difference in comfort, mobility, and long-term vein health.
What Is Venous Stasis Dermatitis?
Venous stasis dermatitis is an inflammatory skin condition caused by chronic venous insufficiency. It occurs when veins in the legs struggle to move blood efficiently back toward the heart. As blood pools in the lower legs, pressure increases within the veins and fluid can leak into nearby tissue.
That fluid buildup triggers inflammation in the skin, leading to visible and often uncomfortable changes. The condition most commonly affects the lower legs and ankles and tends to develop gradually over time.
Venous stasis dermatitis is more common in adults over age 50 and occurs more frequently in women, though it can affect anyone with circulation issues in the legs.
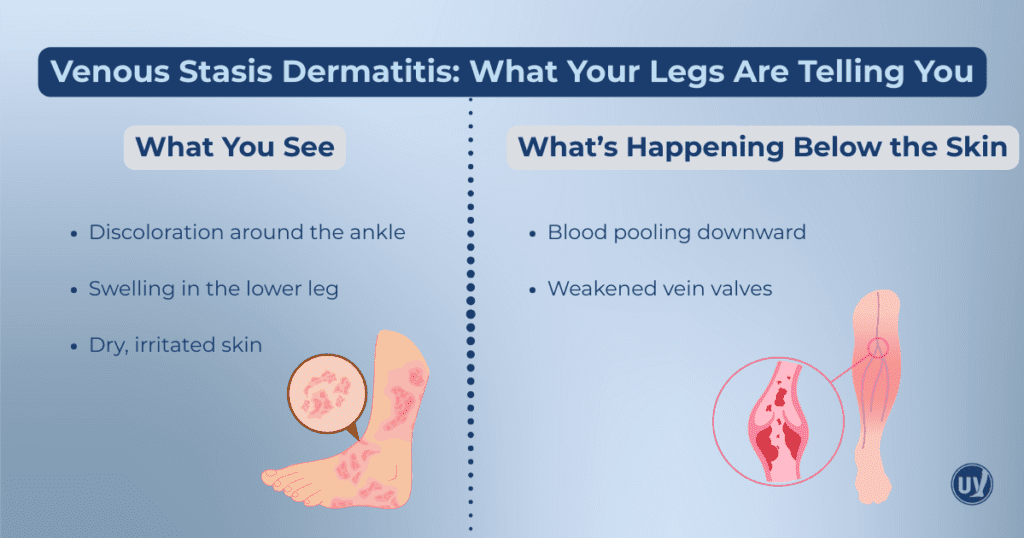
Why Poor Circulation Triggers Skin Changes
Healthy veins rely on one-way valves that keep blood moving upward against gravity. When those valves weaken or fail, blood flows backward and pools in the lower legs. This increased pressure stretches the vein walls and allows fluid, proteins, and blood cells to escape into surrounding tissue.
As this process continues, the skin becomes inflamed and fragile. Oxygen and nutrients have a harder time reaching the area, slowing healing and increasing the risk of infection or ulceration.
Venous stasis dermatitis is often one of the first visible warning signs that circulation in the legs is compromised.
Stages of Venous Stasis Dermatitis
Venous stasis dermatitis does not appear overnight. It develops in stages, and symptoms can worsen if the underlying vein disease is left untreated.
Early Stage
In the early phase, symptoms may be subtle and intermittent. Common signs include mild swelling around the ankles, itchiness, dry skin, and redness that may resemble eczema. Many people mistake these early symptoms for allergies or irritation.
Moderate Stage
As circulation problems continue, skin changes become more noticeable. Discoloration may develop, often appearing brown, purple, or reddish around the ankles and lower legs. Swelling may persist throughout the day, and the skin can feel tight or uncomfortable.
Advanced Stage
In more advanced cases, the skin becomes fragile and prone to injury. Open sores known as venous ulcers may form, particularly near the ankles. These wounds can be slow to heal and may become painful or infected without proper treatment.
Early evaluation can help slow or prevent progression to more severe stages.
Common Symptoms of Venous Stasis Dermatitis
Symptoms can vary from person to person, but often include a combination of skin changes and circulation-related discomfort.
Common symptoms include:
- Swelling in the legs and ankles
- Persistent itching or burning sensations
- Dry, flaky, or scaly skin
- Skin discoloration, especially brown or purple tones
- Thickened or hardened skin over time
- Open sores or ulcers near the ankles
- Leg heaviness or aching that worsens with standing
These symptoms often improve when legs are elevated and worsen after long periods of sitting or standing.
Most Common Causes of Venous Stasis Dermatitis
Venous stasis dermatitis develops due to conditions that impair blood flow in the legs. While several factors can contribute, most cases share a common link to poor circulation.
Chronic Venous Insufficiency
This is the primary cause of venous stasis dermatitis. Faulty vein valves allow blood to pool in the legs, increasing pressure and triggering skin inflammation.
Varicose Veins
Enlarged, twisted veins are a visible sign of valve failure. Varicose veins increase the risk of chronic venous insufficiency and related skin changes.
Deep Vein Thrombosis
A history of blood clots in the deep veins can damage vein valves and disrupt normal circulation, increasing long-term risk.
Obesity
Excess weight places additional pressure on leg veins, making it harder for blood to flow upward efficiently.
Congestive Heart Failure
Heart conditions that affect circulation can contribute to fluid buildup in the legs and worsen venous pressure.
High Blood Pressure
Elevated blood pressure can strain blood vessels and impact overall vascular health.
While these are common causes, venous stasis dermatitis often results from a combination of risk factors rather than a single issue.
How a Vein Specialist Helps Manage Venous Stasis Dermatitis
Treating venous stasis dermatitis effectively requires addressing the underlying vein disease, not just the skin symptoms. A vein specialist evaluates circulation in the legs using imaging and clinical assessment to determine what is driving the condition.
Treatment plans may include:
- Managing faulty veins to improve blood flow
- Reducing pressure in the lower legs
- Supporting skin healing and comfort
- Recommending compression therapy when appropriate
- Providing guidance on daily habits that support circulation
By improving venous function, inflammation decreases and the skin has a better chance to heal and stay healthy.
Why Early Treatment Makes a Difference
Venous stasis dermatitis is a progressive condition. Without proper care, symptoms tend to worsen over time and can lead to complications like chronic ulcers or infections.
Early treatment can help:
- Reduce swelling and discomfort
- Improve skin appearance and texture
- Lower the risk of ulcers
- Support long-term circulation health
- Improve daily comfort and mobility
Seeking care sooner rather than later often leads to better outcomes and fewer disruptions to daily life.
Frequently Asked Questions
While it appears on the skin, venous stasis dermatitis is caused by underlying vein disease. Treating circulation issues is key to managing symptoms and preventing progression.
Symptoms may temporarily improve with leg elevation or compression, but the condition typically does not resolve without addressing the underlying venous insufficiency.
Yes. Venous ulcers can be slow to heal and increase the risk of infection. Early evaluation and proper treatment are important to prevent complications.
Take the Next Step Toward Healthier Legs
Venous stasis dermatitis can be uncomfortable, frustrating, and disruptive, but it does not have to control your life. With proper evaluation and expert care, symptoms can be managed and circulation can improve.
The specialists at United Vein & Vascular Centers understand how vein disease affects both comfort and confidence. They work closely with patients to identify the cause of venous stasis dermatitis and develop personalized treatment plans designed to reduce symptoms, improve mobility, and support long-term vein health.
Contact UVVC today and take the first step toward healthier skin and better circulation today.