Blood clots in the legs are more than just uncomfortable, they can be dangerous. Understanding what causes them and how vascular issues contribute is crucial for preventing serious complications. This guide will help you learn the risk factors, symptoms, and why consulting a vein specialist is often the safest step.
What Are Blood Clots?
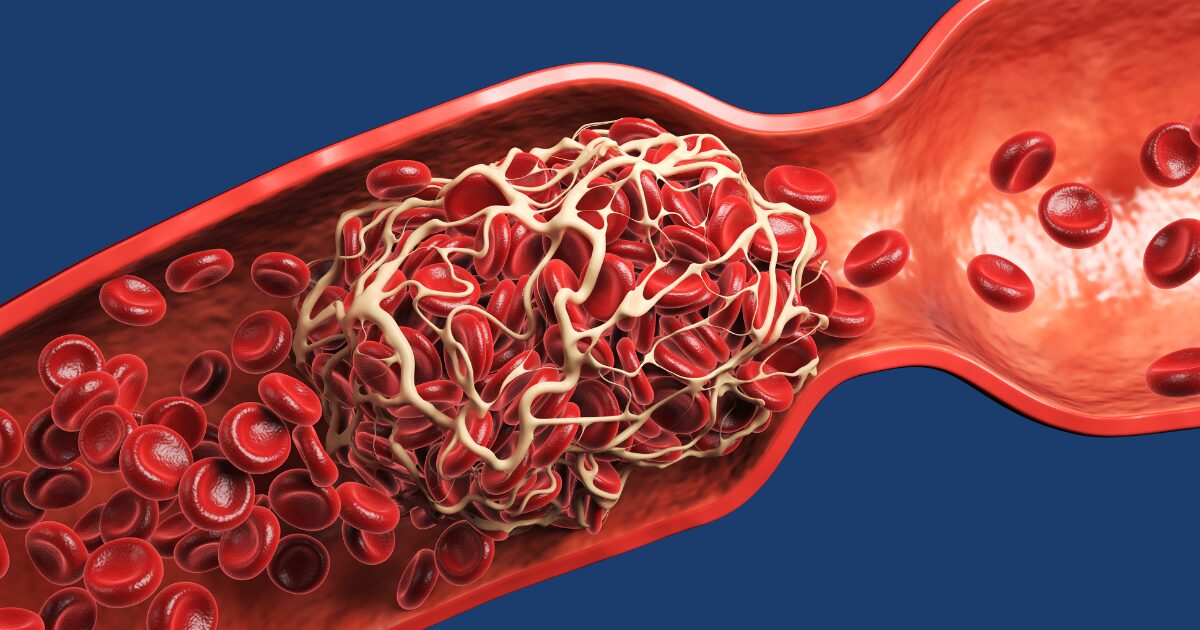
A blood clot, medically known as a thrombus, occurs when blood changes from a liquid to a semi-solid or solid state. This process is a natural defense mechanism. For example, if you cut yourself, clotting prevents excessive blood loss and supports healing.
However, blood clots that form inside your veins or arteries can disrupt normal blood flow. When a clot develops in the deep veins of the legs, it is called deep vein thrombosis (DVT). Left untreated, a DVT can lead to severe complications, including a pulmonary embolism, where the clot travels to the lungs, a potentially life-threatening condition.
Why Do Blood Clots Form in the Legs?
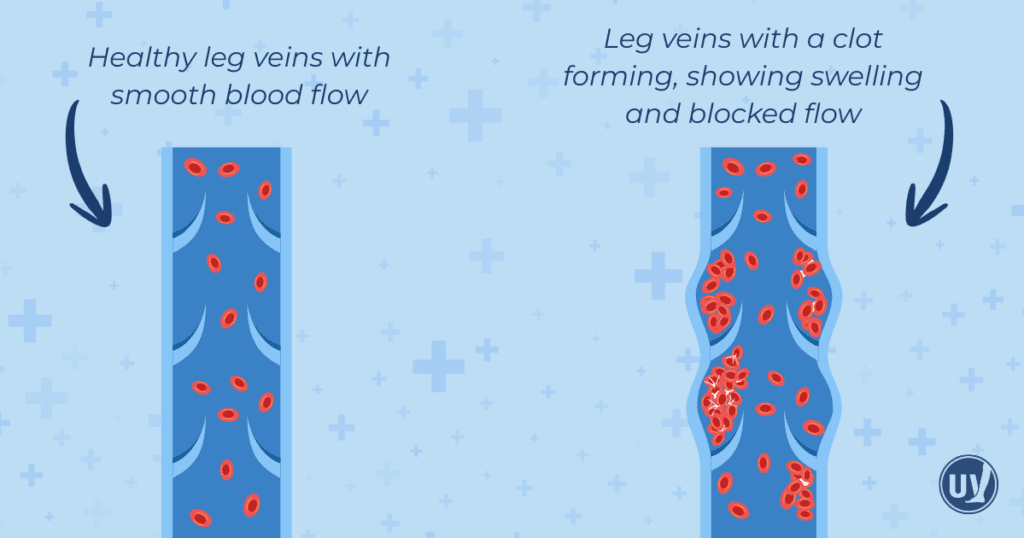
Several factors can make you more susceptible to blood clots, especially in the legs. Blood clots form when the normal flow of blood is slowed or disrupted, when your blood becomes more likely to coagulate, or when your vein walls are damaged.
Common Causes of Blood Clots in Legs
- Slow or Stagnant Blood Flow: Sitting or standing for long periods can reduce circulation, allowing blood to pool and clot. Long flights, desk jobs, or prolonged recovery from surgery can all increase risk.
- Vein & Vascular Conditions: Certain vein and artery problems can raise the likelihood of clot formation:
- Varicose veins: Enlarged, twisted veins can slow blood flow, making clot formation more likely.
- Peripheral artery disease (PAD): Narrowed arteries can reduce blood flow to the legs.
- Atherosclerosis: Hardening of the arteries can trigger clot development.
- Carotid artery disease: Plaque build-up in major arteries can indirectly affect circulation.
- Injury or Trauma: Leg injuries that damage blood vessels or surrounding tissue can trigger clotting as part of the healing process.
- Medical Conditions and Lifestyle Factors
- Obesity
- Smoking
- Heart disease
- Cancer
- Hormone therapy or pregnancy
- Genetic Factors: Inherited clotting disorders, such as Factor V Leiden or prothrombin gene mutation, can make your blood more likely to clot.
Symptoms of Blood Clots in Legs
Recognizing a blood clot early is critical. Symptoms can vary but may include:
- Swelling in one leg, often around the calf or thigh
- Pain or tenderness, sometimes described as cramping
- Red or discolored skin on the leg
- Warmth in the affected area
It’s important to note that some blood clots may form without noticeable symptoms, which is why risk awareness and preventative care are so important.
Preventing Blood Clots in the Legs
You can take steps to reduce your risk of developing blood clots:
- Stay Active: Walk regularly, flex your calves, and avoid prolonged sitting.
- Maintain a Healthy Weight: Excess weight increases pressure on your leg veins.
- Avoid Smoking: Tobacco contributes to vascular damage and clot formation.
- Wear Compression Stockings: For those with varicose veins or prolonged standing, these can improve blood flow.
- Follow Medical Advice After Surgery or Injury: Early movement and prescribed medications can prevent post-operative clots.
When to Seek Medical Help
If you experience sudden leg swelling, pain, redness, or warmth, contact a medical professional immediately. Blood clots can become life-threatening if they travel to the lungs or heart.
Specialists in vein and vascular health can perform tests such as:
- Duplex ultrasound: Non-invasive imaging to detect clots in your veins
- Venography: Imaging that uses contrast dye to view veins
- Blood tests: To check for clotting disorders
Early evaluation and treatment improve outcomes and prevent complications.
Frequently Asked Questions
Yes, varicose veins can slow blood flow and increase the risk of clot formation. While not all varicose veins cause clots, they are an important risk factor to monitor.
Treatment depends on severity. Options include blood thinners, compression therapy, minimally invasive procedures to improve vein flow, or in severe cases, surgical intervention.
Yes. Staying active, maintaining healthy circulation, and consulting a vein specialist for risk assessment can significantly reduce your chances of developing clots.
Contact United Vein & Vascular Centers
You do not have to live with the uncertainty or discomfort of vein problems. At United Vein & Vascular Centers, our specialists provide:
- Comprehensive vein evaluations
- Personalized treatment plans
- Minimally invasive procedures with fast recovery
- Education on how to prevent future blood clots
Take the first step toward healthier legs and better vascular health. Contact United Vein & Vascular Centers today to schedule a consultation and learn how we can help reduce your risks and improve your quality of life.