Contents
- Understanding Post-Surgical Lymphedema
- Why Early Detection Matters
- Recognizing the Signs and Symptoms
- Who Is at Risk? Key Risk Factors
- Essential Steps for Post-Surgical Lymphedema Prevention
- Lymphedema Care: What to Do If You Notice Swelling
- Building a Personalized Lymphedema Management Plan
- Frequently Asked Questions
- Empowering Your Recovery Journey
Post-surgical lymphedema is a condition that can affect many patients after surgery. It involves swelling due to lymph fluid buildup, often in the arms or legs. This condition can be distressing, but understanding it is the first step toward prevention.
Early detection and care are crucial in managing post-surgical lymphedema. Recognizing the signs early can lead to better outcomes and improved quality of life. Patients and caregivers should be aware of the symptoms and risk factors.
Lymphedema care involves a combination of strategies, including exercise, skin care, and compression therapy. These measures can help reduce swelling and prevent complications. It’s important to work closely with healthcare providers to develop a personalized care plan.
Education and awareness are key to preventing post-surgical lymphedema. Patients should be informed about the condition before surgery and know what to watch for afterward. By staying informed and proactive, patients can take control of their recovery journey.
Understanding Post-Surgical Lymphedema
Lymphedema, particularly post-surgical, involves swelling due to an accumulation of lymph fluid. This fluid builds up when the lymphatic system is disrupted, often during surgery. Post-surgical lymphedema commonly affects areas where lymph nodes are removed or vessels damaged.
The lymphatic system is vital for maintaining fluid balance and immune function. Surgery that alters this system can hinder lymph fluid drainage, leading to swelling. This condition can develop immediately after surgery or even months to years later.
Symptoms can include persistent swelling, a feeling of heaviness, and tightness in the affected area. Skin changes, such as thickening or hardening, may also occur. These symptoms should be monitored closely to prevent further complications.
Understanding the nature of lymphedema helps in its effective management. Key points to remember include:
- Swelling in limbs.
- Decreased flexibility.
- Changes in skin texture.
Awareness of these symptoms allows for timely intervention and improved outcomes. By staying informed, patients can take proactive steps in their recovery and quality of life management.
Why Early Detection Matters
Detecting lymphedema early is crucial for effective intervention. Timely detection allows for more effective management and can prevent complications. The earlier you act, the better your chances of controlling the condition.
When symptoms are caught early, they can often be managed with non-invasive techniques. These may include compression therapy and gentle exercises. Early intervention not only controls symptoms but also preserves quality of life.
One of the most effective strategies involves regular monitoring for any signs of swelling or discomfort. Having a keen awareness of your body’s changes plays a vital role. This proactive approach can lead to prompt medical advice and treatment.
Consider these early signs to look out for:
- Unexplained swelling.
- Persistent heaviness.
- Changes in skin texture.
By understanding the importance of early detection, patients can take an active role in their health. Acting swiftly when symptoms first appear can make a significant difference in outcomes and overall wellbeing.
Recognizing the Signs and Symptoms
Identifying lymphedema symptoms early can make a crucial difference in managing the condition. Common indicators often begin subtly but grow noticeable over time. Awareness is key to taking prompt action.
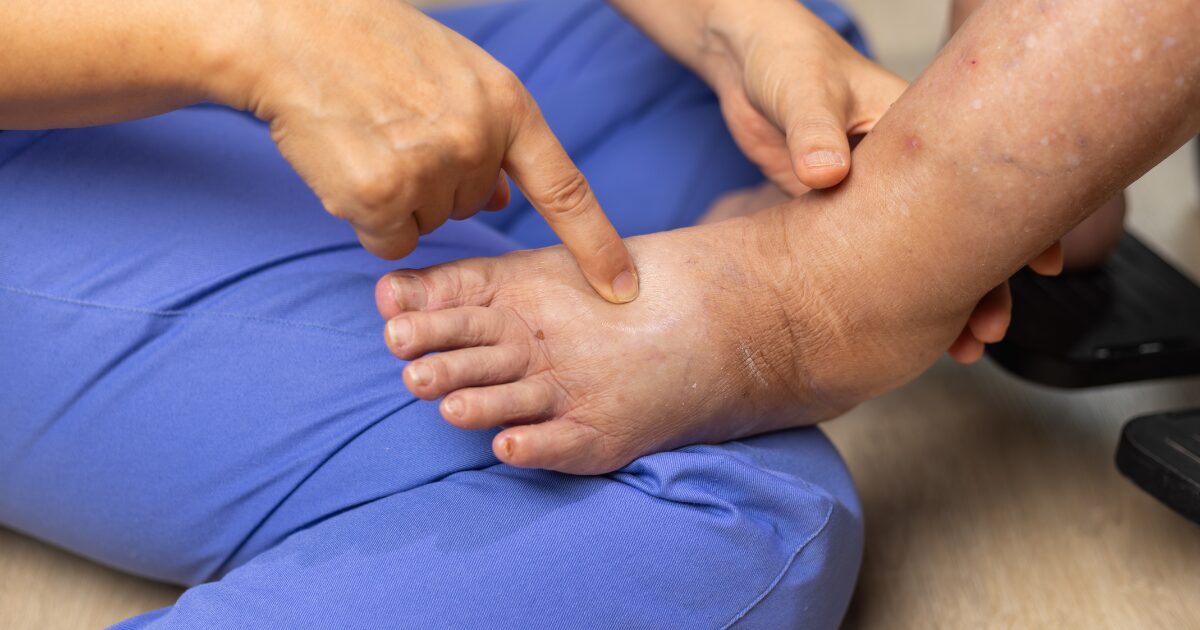
Swelling in the affected area is the most recognizable sign. You might observe it after physical activity or as the day progresses. The swelling is often accompanied by other physical changes.
Beyond swelling, you may also feel a heaviness or tightness. This can occur in the limb affected by the lymph buildup. Such feelings can affect your daily activities and mobility.
Keep an eye out for these additional signs:
- A feeling of fullness.
- Decreased flexibility.
- Thickening or hardening of the skin.
Being observant and noting changes allows for early medical intervention. If these symptoms are familiar, consult your healthcare provider for an evaluation. Early recognition and action pave the way for effective lymphedema management.
Who Is at Risk? Key Risk Factors
Post-surgical lymphedema does not affect everyone equally. Understanding who is at risk helps in prevention and early intervention. Certain factors increase susceptibility to this condition.
Individuals undergoing extensive surgery may find themselves more at risk. This is especially true if lymph nodes are removed or damaged. Radiation therapy following surgery further elevates this risk.
Additional factors include:
- Existing infections.
- Cancer patients, particularly breast cancer.
- Previous history of lymphedema.
Recognizing these risk factors allows patients to be proactive about their health. It emphasizes the need for informed discussions with vascular specialists.
Essential Steps for Post-Surgical Lymphedema Prevention
Taking steps to prevent post-surgical lymphedema is vital for a smoother recovery. Early action ensures better management of potential symptoms. Here’s how you can be proactive.
First, understanding the importance of gentle exercises cannot be overstated. Light activity aids lymphatic flow and diminishes swelling. It’s beneficial to follow a tailored exercise plan provided by your healthcare team.
Second, proper skin care routines can significantly reduce risk. Keeping the skin clean and moisturized prevents infections. Minor infections can exacerbate lymphedema, so vigilance is key.
- Use gentle cleansers.
- Apply moisturizer daily.
- Avoid cuts and scratches.
Wearing compression garments offers another layer of protection. These garments apply necessary pressure, reducing fluid buildup. Speak to a specialist about the right type and fit for you.
Incorporating a balanced diet and maintaining a healthy weight supports your lymphatic system. Proper nutrition helps the body heal and reduces lymphedema risk.
- Focus on whole foods.
- Hydrate adequately.
- Avoid excessive salt.
Finally, staying informed and self-aware equips you for quick action. Recognize early symptoms and consult healthcare providers promptly. Awareness and timely response can make all the difference.
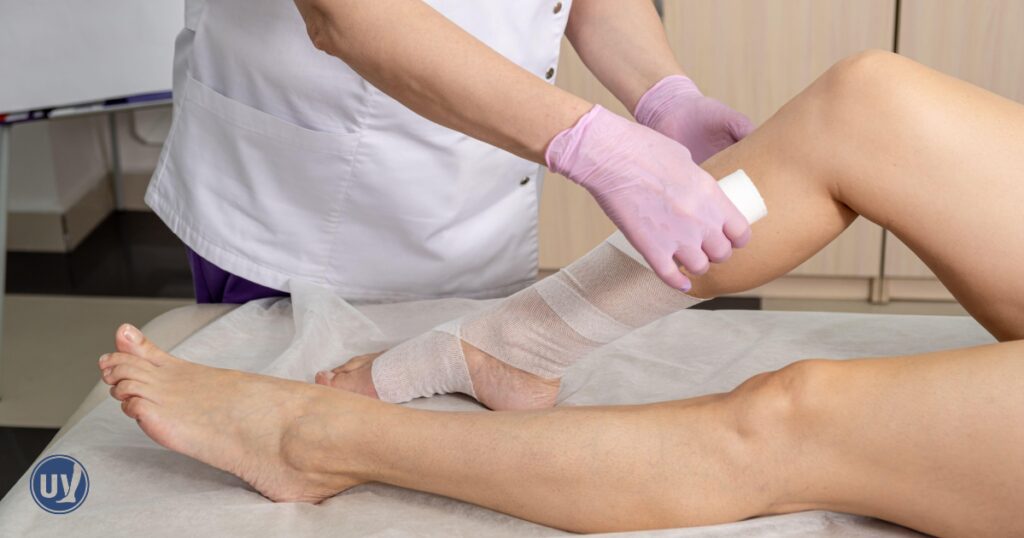
Lymphedema Care: What to Do If You Notice Swelling
If you observe swelling post-surgery, it’s crucial to act swiftly. Early intervention can prevent further complications. Begin by contacting your healthcare provider to discuss your symptoms.
Manual lymphatic drainage, a specialized massage technique, may be beneficial. This method helps move excess lymph fluid and reduce swelling. Always seek a professional skilled in this type of therapy.
Compression therapy is another effective treatment. Wearing compression garments may help alleviate swelling. Your healthcare provider can advise on the best garment for your condition.
Engaging in appropriate exercises can also assist in managing symptoms. Tailored physical activities enhance lymphatic flow and flexibility. Ensure your routine is approved by a healthcare professional.
Consider these actions if swelling occurs:
- Contact your doctor immediately.
- Inquire about manual lymphatic drainage.
- Discuss compression garment options.
- Follow an exercise regimen.
These steps can lead to better management and improved quality of life. Remember, prompt care is key to managing lymphedema effectively.
Building a Personalized Lymphedema Management Plan
Creating a tailored lymphedema management plan is vital for effective care. Every patient’s condition is unique, so personalized strategies are necessary. Collaboration with your healthcare team ensures a plan that suits your specific needs.
Start by setting realistic goals. These goals should focus on reducing swelling and improving function. Involving your healthcare provider will help you prioritize and achieve these objectives. Your plan may include various therapies.
Regular check-ins with your healthcare team are important. These appointments provide an opportunity to monitor your progress and make necessary adjustments. Open communication will ensure that your management plan remains effective.
Empower yourself by staying informed about your condition. With a personalized plan, you can confidently manage lymphedema and maintain a higher quality of life. Remember, you are not alone on this journey.
Frequently Asked Questions
Post-surgical lymphedema is swelling that occurs when lymph fluid builds up after surgery, often in the arms or legs. It can develop weeks, months, or even years after a procedure.
Catching swelling or subtle changes early allows for prompt interventions—like compression therapy or gentle exercises, which can reduce severity and improve long-term outcomes.
Maintaining mobility, practicing gentle limb care, attending follow-up appointments, and reporting unusual swelling to a healthcare provider can all help minimize the risk of post-surgical lymphedema.
Empowering Your Recovery Journey
Post-surgical lymphedema can feel challenging, but early detection and proactive care make a meaningful difference. You don’t have to navigate it alone, support and guidance are available.
Partner with the experts at UVVC to create a personalized recovery plan that protects your health, reduces swelling, and improves your quality of life. Schedule a consultation at your local vascular clinic today and take the next step toward a stronger, healthier recovery.