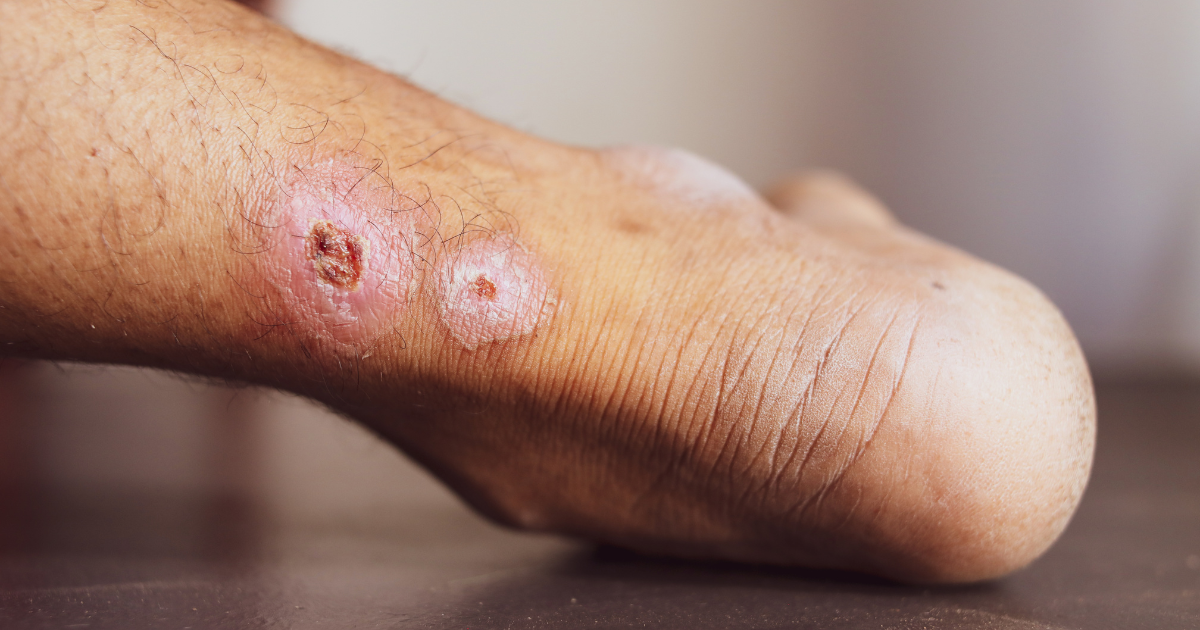
Venous ulcers may start as a small, persistent sore, but they can signal a serious underlying vein problem. These ulcers are caused by damaged or weakened veins, often linked to chronic venous insufficiency. While they are most common near the ankles, they can occur anywhere in the lower legs.
In the United States, venous ulcers affect about 3 in 1,000 adults. Early detection is key to preventing prolonged discomfort, infection, and chronic complications. If you notice unusual sores, swelling, or changes in your legs, understanding the signs of venous ulcers is essential.
What Are Venous Ulcers?
A venous ulcer is a sore on the skin caused by improper blood flow in the veins. When veins fail to return blood efficiently from the legs to the heart, pressure builds up in the lower extremities. This pressure weakens the skin and underlying tissue, leading to ulcer formation.
Unlike ulcers associated with the digestive system, venous ulcers appear externally. They are often shallow, red, and accompanied by swelling, itching, or discomfort. Over time, untreated ulcers can become chronic, slow-healing wounds that significantly impact mobility and quality of life.
Common Causes of Venous Ulcers
Understanding why venous ulcers develop can help you take preventive steps. The most common causes include:
- Chronic venous insufficiency (CVI): A condition where veins are unable to efficiently return blood to the heart. CVI is the most frequent cause of venous ulcers.
- Varicose veins: Twisted, enlarged veins that impair circulation and increase pressure in the legs.
- Previous leg injuries or surgeries: Trauma can weaken veins and contribute to ulcer development.
- Obesity or excess weight: Increased pressure on the veins makes ulcers more likely.
- Prolonged standing or sitting: Jobs or lifestyles that limit leg movement can lead to venous stasis.
- Age and genetics: Family history and older age are risk factors.
Even if you only have minor vein issues, being aware of these risks can help you take action before ulcers develop.
Early Warning Signs to Watch For
Venous ulcers often begin subtly, but early recognition is critical. Signs may include:
- Persistent swelling in the lower legs or ankles
- Skin discoloration: The skin may appear brown, reddish, or dark purple
- Sores that won’t heal: Small abrasions that persist longer than two weeks
- Shiny or tight skin on the lower legs
- Leg heaviness or aching, especially after standing for long periods
- Itching or irritation around the affected area
If you notice any of these symptoms, don’t wait. Early evaluation by a vein specialist can prevent the ulcer from worsening.
The Risks of Ignoring Venous Ulcers
Leaving venous ulcers untreated can have serious consequences:
- Infection: Open ulcers are prone to bacterial infection, which can cause increased swelling, redness, and pain. Severe infections can enter the bloodstream, leading to systemic issues.
- Chronic pain: Persistent ulcers often result in discomfort or aching in the lower legs, interfering with daily life.
- Delayed healing: Poor circulation makes it difficult for the body to repair damaged skin. Ulcers may remain open for months without proper treatment.
- Skin changes: Untreated ulcers can lead to thickened, hardened skin and further vein damage.
These risks underscore the importance of professional care.
How Venous Ulcers Are Evaluated
At United Vein & Vascular Centers, evaluation begins with understanding whether an underlying vein or vascular condition may be contributing to leg symptoms or skin changes.
Medical history review: Discussing previous vein issues, symptoms, risk factors, and changes in the skin or lower legs
Physical exam: Looking for signs of vein disease, swelling, skin discoloration, or other circulation-related concerns
Ultrasound imaging: Evaluating blood flow in the legs and identifying vein abnormalities, such as venous reflux
This comprehensive approach helps determine whether vein disease may be playing a role and supports a treatment plan focused on the underlying circulation issue.
Treatment Options for Venous Ulcers
Treatment focuses on addressing both the ulcer and the underlying vein problem. Options include:
1. Compression Therapy
Compression stockings can help support circulation, reduce swelling, and manage symptoms related to venous insufficiency.

2. Minimally Invasive Vein Treatments
Procedures such as radiofrequency ablation (RFA), VenaSeal™, Varithena®, ultrasound-guided sclerotherapy, or microphlebectomy may be recommended to treat damaged veins and help blood reroute through healthier veins.
4. Ongoing Vein and Vascular Management
A vein specialist can help monitor circulation concerns, recommend appropriate treatment options, and coordinate next steps when additional care is needed.
A personalized care plan focuses on addressing the underlying vein disease that may contribute to venous ulcers, while patients with active wounds may also need care from a dedicated wound care provider.
Często zadawane pytania
Healing time varies based on severity, circulation, and treatment. Minor ulcers may heal in a few weeks with proper care, while chronic ulcers can take several months.
Yes. Pain can range from mild aching to sharp discomfort, especially when standing or walking. Effective treatment can significantly reduce pain and swelling.
Many venous ulcers can be prevented by managing vein health. Wearing compression stockings, exercising, and addressing varicose veins early reduce risk. Regular monitoring is essential.
Take Action: Seek Expert Care at United Vein & Vascular Centers
Venous ulcers can be a serious complication of underlying vein disease, but identifying circulation problems early can help patients better understand their symptoms and take the next step in care. Professional evaluation, appropriate vein treatment, and lifestyle adjustments may help support long-term vein health and reduce the risk of worsening symptoms.
The vein specialists at UVVC provide personalized care for vein and vascular conditions that may contribute to venous ulcers. Their comprehensive approach is designed to:
- Help identify underlying circulation issues
- Reduce symptoms such as leg swelling, heaviness, and discomfort
- Support improved mobility and daily comfort
- Protect long-term vein health
If you’re concerned about venous ulcers, skin changes, or ongoing leg symptoms, contact United Vein & Vascular Centers today to schedule a consultation and better understand your treatment options.Don’t wait. Contact United Vein & Vascular Centers today and take the first step toward healthier, pain-free legs.