Objawy i możliwości leczenia choroby refluksowej żył
If your legs often feel heavy, tired, or achy at the end of the day, you might assume it is just part of getting older...
Read More
Venous reflux, commonly referred to as chronic venous insufficiency (CVI), is a progressive vein condition that can seriously impair your quality of life, but the good news is that modern, in-office, minimally invasive vein treatments can help relieve symptoms and improve circulation.
If you are experiencing any of these symptoms, please contact us today!

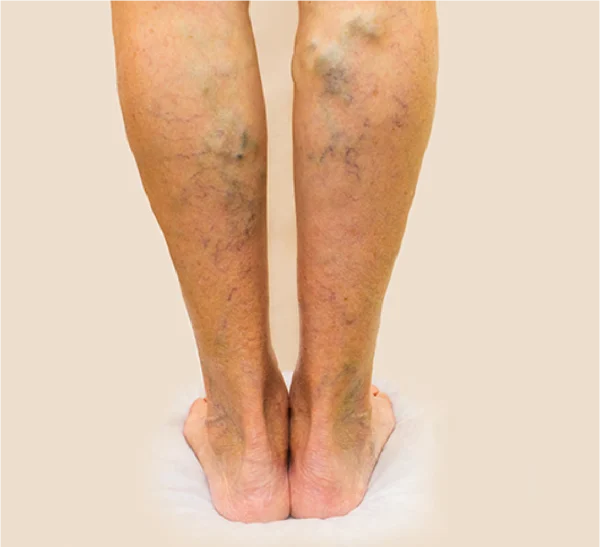
Venous reflux happens when the valves inside your leg veins don’t close properly. Instead of moving blood efficiently toward the heart, blood can flow backward and pool in the legs. Over time, this can raise pressure in the veins and lead to symptoms like aching, heaviness, swelling, varicose veins, and even skin changes or ulcers.
Venous reflux typically develops when vein valves weaken over time. Common contributing factors include:
Your leg veins contain one-way valves that help push blood upward against gravity. With venous reflux, those valves become weakened or damaged, allowing blood to leak backward, increasing vein pressure, stretching vein walls, and can contribute to varicose veins, spider veins, leg swelling, leg ulcers, and RLS.

Venous reflux isn’t just a cosmetic concern. When left untreated, it can worsen over time and lead to more serious complications. Ongoing poor circulation may cause persistent leg swelling and discomfort, skin discoloration or eczema-like irritation, and hardening or thickening of the tissue (known as lipodermatosclerosis).
Some people may also experience superficial vein inflammation, and in more advanced cases, venous ulcers, chronic wounds near the ankles that can be difficult to heal. If you’ve noticed skin changes, ongoing swelling, or a sore that isn’t healing properly, it’s important to have your veins evaluated by a vascular specialist.
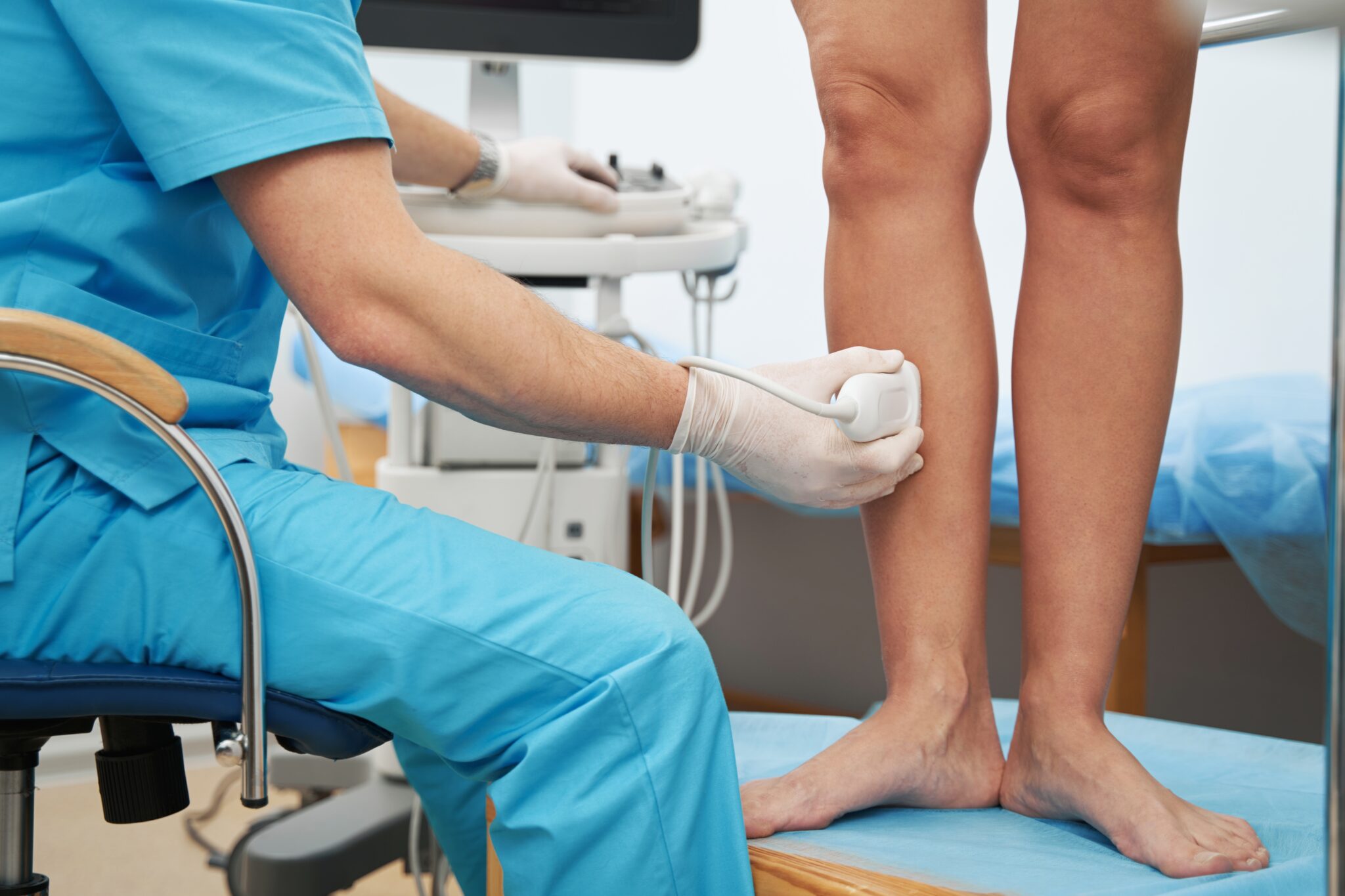
A vein specialist can often suspect reflux based on your symptoms and a physical exam, but confirming it requires imaging.
A venous duplex ultrasound is a noninvasive imaging test that uses sound waves to create pictures of the veins and measure how blood is flowing through them. It combines standard ultrasound with Doppler ultrasound, helping detect problems like blood clots, blockages, and venous reflux and is considered the gold standard for vein testing.
This ultrasound evaluates:
Ultrasound is non-invasive and typically performed right in the office.

Treatment depends on which veins are affected, how severe the reflux is, and your symptoms and goals.
For mild symptoms or as a first step, your provider may recommend:
If reflux is causing significant symptoms or complications, common outpatient options include:
Your provider may use one treatment or a combination, depending on the pattern of reflux and the visible veins.

Most modern vein procedures are performed in an outpatient setting and are minimally invasive, meaning no hospital stay is required. Many treatments can be completed in under an hour and are followed by a relatively short recovery period, allowing patients to return to normal activities quickly. After treatment, many people report noticeable improvements such as less leg heaviness or aching, reduced swelling, and greater comfort during daily activities. When visible veins are treated, patients may also experience less irritation and an improved appearance of prominent veins.

Consider scheduling an evaluation if you have:
It often feels like heaviness, aching, throbbing, swelling, burning/itching, restlessness or fatigue in the legs, especially after standing or sitting for long periods.
Not exactly. Venous reflux is a valve problem that can cause varicose veins. Varicose veins are a common visible result of reflux, but you can have reflux even without obvious bulging veins.
Usually, no. Lifestyle changes and compression may reduce symptoms, but they don’t repair damaged valves. If symptoms progress, medical treatment may be recommended.
A venous duplex ultrasound evaluates blood flow and valve function to confirm reflux and map which veins are affected.
Most procedures are done with local numbing and are generally well tolerated. Your care team will explain what to expect based on the recommended approach.
It will worsen over time and may lead to increasing pain/swelling, skin changes, and venous ulcers.